Glaucoma
Hydrus Microstent
Help control your eye pressure and possibly reduce your need for medication with the Hydrus Microstent
- Hydrus is roughly the size of an eyelash.
- 77% of Hydrus Microstent patients saw a significant reduction in eye pressure*
- 78% of all patients with a Hydrus Microstent were drop free at 2 years*
View more details on the Ivantis website.
*Samuelson TW, Chang DF, Marquis R, et al; HORIZON Investigators. A Schlemm canal microstent for intraocular pressure reduction in primary open-angle glaucoma and cataract: The HORIZON Study. Ophthalmology. 2019;126:29-37.


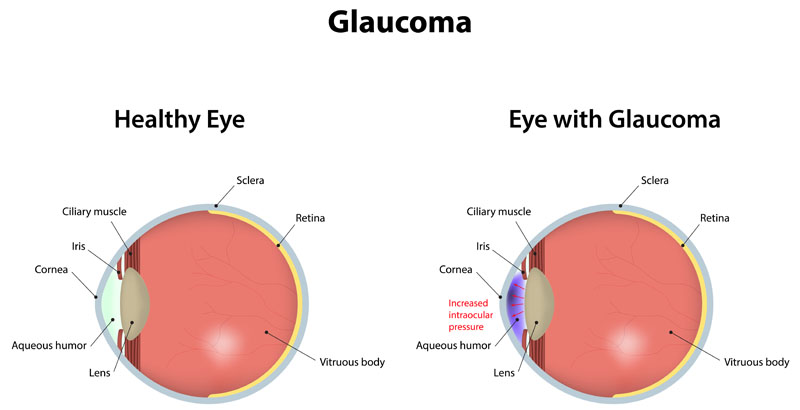
Glaucoma refers to a group of diseases that cause damage to the optic nerve. Containing more than a million nerve fibers, the optic nerve connects the eye to the brain. This important nerve is responsible for carrying images to the brain. The optic nerve fibers make up a part of the retina that gives us sight. This nerve fiber layer can be damaged when the pressure of the eye (intraocular pressure) becomes too high. Over time, high pressure causes the nerve fibers to die, resulting in decreased vision. Vision loss and blindness will likely result if glaucoma is left untreated.
Symptoms:
Glaucoma has been nicknamed the “sneak thief of sight” because it often goes undetected and causes irreversible damage to the eye. There are usually no symptoms in the early stages of the disease. Many people have glaucoma but are not aware of it. As the disease progresses, vision seems to fluctuate and peripheral vision fails. If left untreated, vision can be reduced to tunnel vision and eventually, total blindness.
Causes:
Glaucoma usually occurs when fluid in the eye builds up, causing higher pressure than the eye can withstand. The canal responsible for draining this fluid becomes plugged, preventing proper drainage. In other cases, the eye may produce more fluid than normal and simply cannot be drained fast enough, producing higher intraocular pressure. Researchers do not know exactly what makes some people more prone to this problem. Other causes may include trauma, genetic disorders and low blood flow to the optic nerve.
Risk Factors:
Having high intraocular pressure increases the risk of developing glaucoma. Those who are over forty years of age and who are African-American also have an increased risk. Anyone sixty years of age is more at risk, especially Mexican-Americans. Furthermore, those with a family history of glaucoma are at higher risk of developing glaucoma. Having systemic diseases such as diabetes, high blood pressure and heart problems also increase your risk. Other risk factors include nearsightedness or poor distance vision and direct trauma to the eye.
Types:
There are two major types of glaucoma: chronic, or primary open-angle glaucoma (POAG), and acute closed-angle glaucoma.
- Chronic: Open-angle glaucoma damages the eye with no warning signs. It is the most common type of glaucoma and is often referred to as the “silent type.” Damage occurs over time, usually without notice.
- Acute closed-angle glaucoma: Closed-angle glaucoma happens quickly. An “attack” may produce a red, painful eye and symptoms such as facial pain, headache, blurry vision, rainbow-colored haloes around lights, nausea and vomiting. It is a severe medical emergency.
Diagnosis:
The region’s only fellowship trained glaucoma specialists may use tonometry or gonioscopy to test for glaucoma.
- Tonometry: A key test in glaucoma diagnosis is tonometry. A tonometer measures eye pressure, better known as intra-ocular pressure.
- Gonioscopy: Gonioscopy may be performed to look at the angle of the eye to detect if it is open or closed. An inspection of the health of the optic nerve is also important in assessing any damage that may have occurred because of glaucoma. If damage is suspected, the doctor may measure your overall visual field with a computerized perimeter or analyze your nerve fiber layer with scanning laser ophthalmoscopy.
Treatment:
The goal of glaucoma treatment is to reduce eye pressure to a level at which no more damage occurs. Treatment is given in the form of prescription eye drops and occasionally, oral-systemic drugs. Laser treatment has been shown to work just as well as medicines to prevent more damage from occurring. In certain cases in which medication or laser procedures do not achieve this goal, surgery is helpful. Many times therapy includes a combination of these treatments. It is important to understand that glaucoma cannot be cured, but can be controlled. Unfortunately, vision loss caused by glaucoma cannot be reversed.
Minimally Invasive Glaucoma Surgery
Minimally Invasive Glaucoma Surgery (MIGS), when used during Glaucoma Surgery, has been shown to lower pressures and reduce the patients dependence on drops.

